Can a brain scan reveal whether someone has depression?
It’s a question researchers have been asking for years. Changes in brain structure have been observed in people with depression, raising hopes that MRI scans might one day help doctors diagnose or better understand the condition.
In a new international study led by researchers at The University of Queensland’s Institute for Molecular Bioscience (IMB), scientists tested just how far that idea can go.
The answer? Brain scans hold some clues — but they’re not a diagnostic tool.
Training computers to read the brain
The team analysed MRI brain scans from nearly 8,000 people in the UK Biobank, including around 1,500 people with a history of major depressive disorder.
Using advanced computer modelling, they trained algorithms to look at tiny three-dimensional units in the brain called voxels, the 3D equivalent of pixels, across the brain’s grey matter. The goal was to see whether patterns in brain structure could distinguish people with depression from those without it.
One model, based on a well-established machine-learning method, performed better than chance. People with depression were more likely to receive higher predicted risk scores from the brain-based model.
However, the accuracy was modest.
“Our results show that grey matter structure does carry information about depression,” said lead author Dr Jiayue-Clara Jiang. “But that information is limited. Brain structure alone is not enough to accurately diagnose depression.”
Interestingly, a more complex deep-learning approach; often seen as the cutting edge of artificial intelligence, did not perform better than the simpler method.
A complex condition with many causes
Depression is one of the leading causes of disability worldwide. But it doesn’t have a single biological cause. Genetics, life experiences, stress, environment and physical health all play a role.
The researchers found that the brain-based prediction overlapped partly with genetic risk for depression. When combined with a genetic risk score, prediction improved slightly — but still not to a level that would be useful in the clinic.
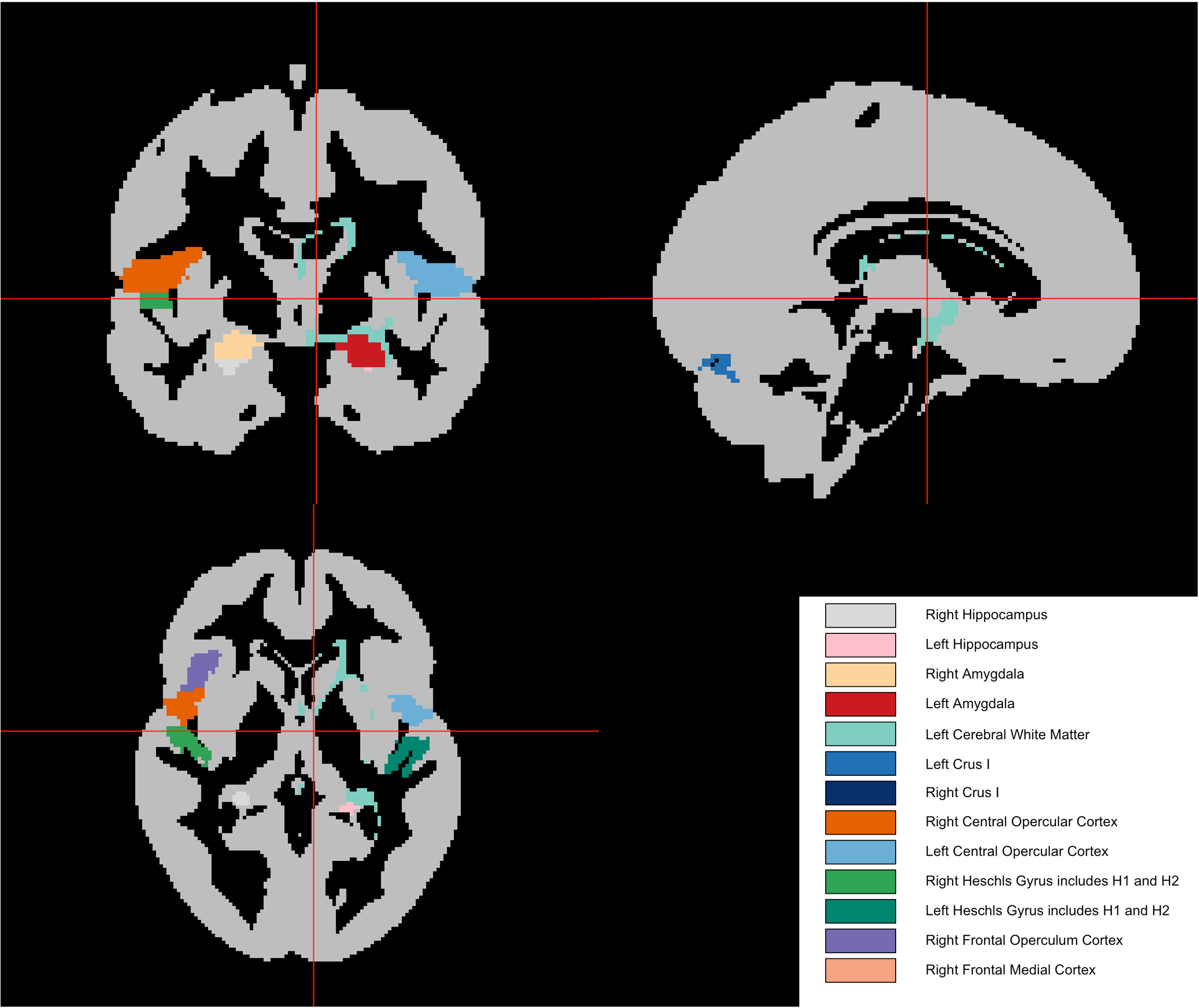
The team also examined which brain regions contributed most to the prediction. Areas such as the hippocampus and amygdala — regions previously linked to mood and emotion — showed signals consistent with earlier research. However, no single brain region stood out strongly enough to act as a clear marker on its own.
Why this matters
While the findings may not deliver a brain scan test for depression, they provide something equally important: clarity.
There has been growing excitement around the idea that artificial intelligence could identify mental health conditions from brain imaging. This study suggests that, at least using current MRI methods and grey matter structure alone, there are clear limits.
The researchers estimate that MRI imaging of grey matter structure explains only about six per cent of the variation in depression risk in this dataset. That means even with larger studies, there is likely a ceiling on how accurate structural MRI-based prediction can become.
“This doesn’t mean brain imaging isn’t valuable,” Dr Jiang said. “It helps us understand the biology of depression and how genetic and environmental factors may affect the brain. But it also tells us we need to look beyond grey matter structure if we want better prediction.”
Future research may explore other types of brain imaging, such as measures of white matter integrity or brain activity, which could capture different aspects of how depression affects the brain.
A research tool, not a diagnostic test
For now, diagnosing depression remains based on symptoms and clinical assessment, not brain scans.
But studies like this help researchers better understand how depression affects the brain and how biology, genetics and life experiences interact.
By setting realistic expectations and identifying the limits of current technology, the team hopes to guide the next generation of research into more effective ways of studying and ultimately treating depression.
Want to know more? Read the full paper published here.
Acknowledgements
The authors would like to thank the participants of the UK Biobank and the DEP-ARREST CLIN cohorts.
This study is an international effort by researchers from the IMB, QIMR Berghofer Medical Research Institute, Kremlin Bicêtre hospital and Paris Brain Institute, and is funded by Inria (French national institute for research in digital science and technology), who funded an international visit to France for Dr Jiang to learn the deep-learning techniques.
To collaborate with Dr Clara Jiang please reach out directly at j.jiang@uq.edu.au